RCM
How One Clinic Increased Revenue
What’s Included
- How one clinic increased revenue by 45%
- Steps to reduce administrative costs by 30%
- Ways to improve clean claim rates
- How real-time reporting and analytics
- The impact of better patient engagement
- Why switching to a full RCM service model
Featured Post
The Top Denial Reasons by Insurance Payers and How to Boldly Outsmart Them
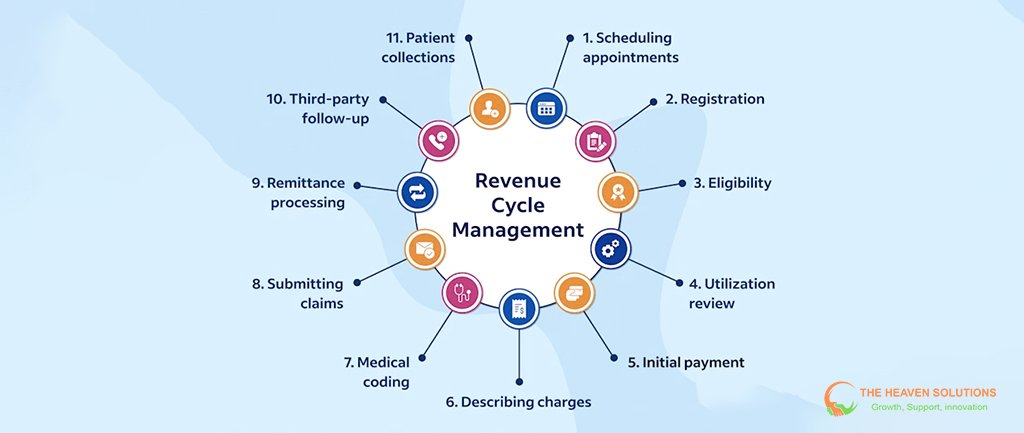
When Dr. Sarah Martinez opened her family practice five years ago, she never imagined she’d be on the brink of closing due to cash flow problems. Fast forward 18 months, and her clinic has increased revenue by 45% while reducing administrative costs by 30%. Her story isn’t unique; thousands of healthcare practices struggle with revenue cycle management inefficiencies that drain profitability and create operational stress.
This real-world case study demonstrates that with the right strategies, technology, and expertise, any healthcare practice can dramatically improve its financial performance without compromising patient care quality. Dr. Martinez’s transformation from a struggling practice to a thriving clinic provides a blueprint that other practices can follow to achieve similar results.
The journey from financial crisis to success involved strategic RCM in medical billing improvements, technology adoption, enhanced patient engagement, and systematic process optimization. Every change was measured, tracked, and refined to ensure maximum impact on the practice’s bottom line.
Understanding the Initial Challenges : Struggle to Success
Dr. Martinez’s practice was experiencing the same problems that plague thousands of healthcare providers across the country. Despite seeing a steady stream of patients and providing excellent clinical care, the practice was hemorrhaging money due to inefficient medical billing RCM processes and operational inefficiencies.
Financial Performance Baseline
The numbers painted a grim picture of the practice’s financial health. With a clean claim rate of just 78%, nearly one in four claims submitted required rework, creating significant delays in payment. The practice’s days in accounts receivable stretched to 65 days, meaning it took over two months to collect payment for services already provided.
The net collection rate of 92% seemed reasonable at first glance, but it meant the practice was leaving 8% of collectible revenue on the table – approximately $48,000 annually for a practice generating $600,000 in charges. The denial rate of 15% was double the industry average, indicating systematic problems in the revenue cycle process.
These poor metrics created a vicious cycle of cash flow problems. With payment delays stretching beyond 60 days, the practice struggled to meet monthly expenses, pay staff, and invest in necessary equipment or improvements.
The Increasing Complexity of Billing and Coding
The practice relied heavily on manual processes that consumed over 40 hours weekly on billing-related tasks. One staff member spent her entire day posting payments, following up on denials, and calling insurance companies for claim status updates. Another team member dedicated significant time to patient billing inquiries and collection calls.
Staff turnover in the billing department compounded these problems. Training new employees on complex RCM systems took weeks, during which productivity dropped and errors increased. The constant turnover meant institutional knowledge was lost, and the same mistakes were repeated by new staff members.
The true cost of these inefficiencies extended beyond just time. Manual processes introduced errors that caused claim denials, delayed payments, and damaged relationships with both payers and patients. Staff morale suffered as team members felt overwhelmed by administrative tasks that kept them from focusing on patient care.
Patient Financial Experience Issues
The practice’s patient collection rate of just 35% revealed serious problems with the patient financial experience. Patients frequently called with questions about their bills, complained about surprise charges, and many simply didn’t pay their balances at all.
The lack of upfront cost transparency meant patients were often shocked by bills they received weeks after their appointments. Without payment plans or flexible options, many patients simply ignored their statements, leading to significant bad debt write-offs.
Patient complaints about billing issues began affecting online reviews and word-of-mouth referrals. The practice’s reputation for clinical excellence was being overshadowed by frustration with billing and financial processes.
Strategic Changes That Made the Difference
Recognizing that the current approach wasn’t sustainable, Dr. Martinez decided to implement a comprehensive transformation strategy. Rather than addressing problems piecemeal, she committed to overhauling the entire revenue cycle management process with expert guidance and proven methodologies.
Revenue Cycle Management Overhaul
The first priority was implementing automated claim scrubbing technology to address the poor clean claim rate. This RCM software automatically checked every claim against hundreds of payer-specific rules before submission, catching errors that previously caused denials.
Real-time eligibility verification was integrated into the patient check-in process. Staff could instantly verify insurance coverage, benefits, and prior authorization requirements before patients were seen, preventing coverage-related denials that had been a major source of delayed payments.
A systematic denial management process replaced the previous reactive approach. Instead of working denials as time allowed, the practice implemented specific protocols for categorizing denials, prioritizing appeals, and tracking resolution progress. Each denial was assigned to a team member with clear timelines for follow-up and appeal submission.
The importance of revenue cycle management became clear as these changes began producing immediate results. Clean claim rates improved from 78% to 85% within the first month, and denial rates dropped from 15% to 11% as systematic errors were eliminated.
Technology Adoption and Integration
The practice upgraded from an outdated, on-premise system to a modern, cloud-based revenue cycle management system that integrated seamlessly with their existing electronic health record. This integration eliminated duplicate data entry and reduced the chance of errors that occurred when information was transferred between systems.
Patient portal implementation gave patients 24/7 access to their billing information and the ability to make payments online. The portal included cost estimation tools that provided patients with accurate out-of-pocket estimates before services were provided.
Automated payment processing reduced the time required to post payments from hours to minutes. Electronic remittance advice (ERA) allowed the practice to receive payment information electronically, and automated posting updated patient accounts in real-time as payments were received.
The revenue cycle optimization achieved through technology adoption freed up significant staff time. The employee who previously spent 40 hours weekly on manual billing tasks could redirect 25 hours toward patient care activities and practice improvement projects.
Patient Engagement and Financial Counseling
A proactive financial counseling program transformed the patient financial experience. Staff were trained to discuss costs upfront, explain insurance benefits in plain language, and offer payment options before services were provided.
Flexible payment plans made healthcare more accessible for patients with larger balances. Instead of requiring full payment at the time of service, the practice offered interest-free payment plans that patients could set up online or by phone.
Cost estimation tools integrated with the practice management system provided accurate estimates based on the patient’s specific insurance benefits. Patients knew their expected out-of-pocket costs before their appointment, eliminating surprise bills and improving satisfaction.
Patient revenue cycle improvements had immediate impact. Upfront collections increased from $2,000 monthly to $8,500 monthly as patients were better prepared for their financial responsibility and had convenient options for payment.
Staff Training and Process Standardization
Comprehensive training ensured that all team members understood their role in the healthcare revenue cycle management process. Instead of having one person responsible for all billing activities, responsibilities were distributed based on each team member’s strengths and interests.
Documented procedures eliminated the institutional knowledge problem that had plagued the practice during staff turnover. Every process was written down with step-by-step instructions, so new employees could become productive quickly without extensive one-on-one training.
Performance metrics tracking helped identify areas where individual team members needed additional support or training. Monthly meetings reviewed key RCM metrics and celebrated improvements while addressing persistent challenges.
Dramatic Improvements Across All Key Metrics
Eighteen months after beginning the transformation process, the results exceeded Dr. Martinez’s expectations. Every key performance indicator showed significant improvement, and the financial impact was substantial enough to secure the practice’s future and fund expansion plans.
Revenue Cycle Performance Gains
The clean claim rate improved from 78% to 95%, meaning 95% of claims were processed without errors and paid within standard timeframes. This improvement alone reduced the administrative burden significantly while accelerating cash flow.
Days in accounts receivable dropped from 65 days to 32 days, cutting the collection timeline in half. This improvement meant the practice was collecting payments for services provided just one month earlier instead of waiting over two months.
The net collection rate increased from 92% to 97%, representing an additional $30,000 annually in collected revenue without seeing more patients or providing additional services. Every percentage point improvement in collection rate translates directly to the bottom line.
The denial rate fell from 15% to 4%, well below the industry average. This improvement reduced the administrative cost of appeals while ensuring more claims were paid on first submission.
Financial Impact and ROI
The combined effect of these improvements resulted in a 45% increase in revenue, adding $180,000 annually to the practice’s collections. This increase came from faster payments, higher collection rates, and reduced write-offs rather than seeing more patients.
Administrative cost reductions of 30% were achieved through automation and improved efficiency. The practice saved approximately $36,000 annually in reduced labor costs while improving accuracy and patient satisfaction.
The return on investment for the technology and process improvements was achieved within six months. The ongoing annual benefit of $216,000 ($180,000 increased revenue plus $36,000 cost savings) far exceeded the initial investment in technology and training.
Operational and Patient Satisfaction Improvements
Patient collection rates improved from 35% to 85% through upfront financial counseling and convenient payment options. This improvement reduced bad debt write-offs by $42,000 annually while improving patient relationships.
Billing inquiries decreased by 60% as patients received clearer statements and had access to their billing information through the patient portal. This reduction freed up front desk staff to focus on patient care and scheduling.
Patient satisfaction scores related to billing and financial processes increased by 25%. Online reviews began highlighting the practice’s transparent billing and convenient payment options as positive differentiators.
Administrative cost reductions of 30% were achieved through automation and improved efficiency. The practice saved approximately $36,000 annually in reduced labor costs while improving accuracy and patient satisfaction.
The return on investment for the technology and process improvements was achieved within six months. The ongoing annual benefit of $216,000 ($180,000 increased revenue plus $36,000 cost savings) far exceeded the initial investment in technology and training.
What Every Practice Can Learn From This Success
Dr. Martinez’s transformation succeeded because of several critical factors that any practice can implement. These success elements provide a framework for other practices seeking similar improvements in their healthcare revenue management.
Stop letting revenue slip through the cracks. Contact The Heaven Solutions today for a free consultation and discover how our partnership can transform your practice’s financial health.
1- Leadership Commitment and Change Management
Dr. Martinez’s transformation succeeded because of several critical factors that any practice can implement. These success elements provide a framework for other practices seeking similar improvements in their healthcare revenue management.
Stop letting revenue slip through the cracks. Contact The Heaven Solutions today for a free consultation and discover how our partnership can transform your practice’s financial health.
2 - Data-Driven Decision Making
Regular monitoring of key performance indicators allowed the practice to track progress and identify areas needing additional attention. Monthly performance reviews became collaborative sessions where the team celebrated successes and problem-solved challenges together.
Benchmark comparisons helped the practice understand how their improvements compared to industry standards and identify opportunities for further optimization. This external perspective ensured that the practice didn’t become complacent with initial improvements.
Revenue cycle analytics revealed patterns and trends that weren’t apparent from individual transactions. For example, the data showed that certain insurance companies had higher denial rates for specific procedure codes, leading to targeted improvements in documentation and coding.
Stop letting revenue slip through the cracks. Contact The Heaven Solutions today for a free consultation and discover how our partnership can transform your practice’s financial health.
3- Strategic Partnership and Expert Guidance
Collaboration with RCM management specialists accelerated improvements and helped avoid common implementation pitfalls. External expertise provided best practices and proven methodologies that would have taken years to develop internally.
Ongoing support and optimization ensured that improvements were sustained and refined over time. Rather than viewing the transformation as a one-time project, the practice established a relationship for continuous improvement.
The external partnership also provided access to advanced technologies and industry insights that weren’t available to individual practices. This access leveled the playing field with larger healthcare organizations that had dedicated revenue cycle management departments.
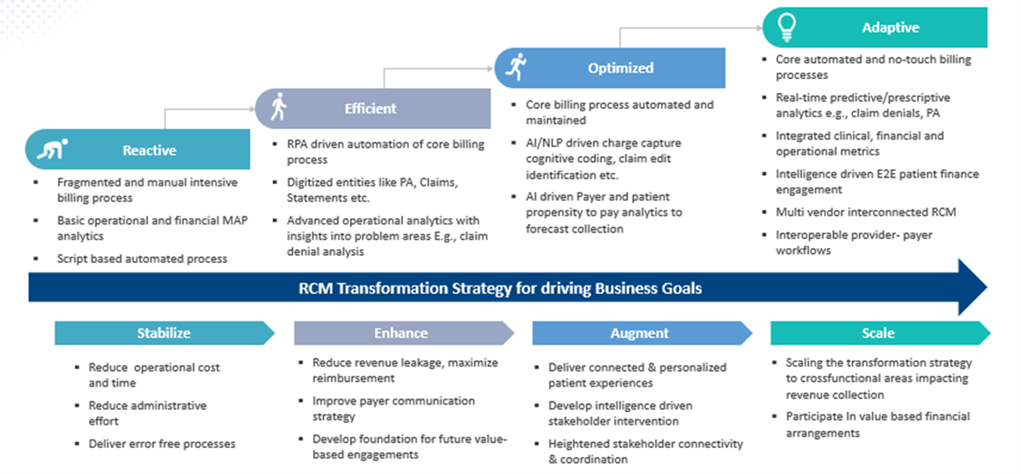
Your Practice Can Achieve Similar Results
Dr. Martinez’s story demonstrates that dramatic financial improvements are possible for practices willing to invest in proven strategies and expert guidance. Her clinic’s transformation from struggling to thriving provides a blueprint that any practice can follow to achieve similar results.
The key lessons from this case study apply to practices of all sizes and specialties. Whether you’re a solo practitioner or part of a multi-physician group, the fundamental principles of effective revenue cycle management remain the same: automate processes, engage patients proactively, and measure performance consistently.
The most important takeaway is that transformation requires commitment to change. Dr. Martinez succeeded because she was willing to invest time, money, and energy in comprehensive improvements rather than looking for quick fixes or partial solutions.
The compound effect of multiple improvements created results that exceeded expectations. Small gains in clean claim rates, collection rates, and operational efficiency combined to produce a 45% revenue increase that secured the practice’s future and enabled expansion plans.
Ready to transform your practice’s financial performance like Dr. Martinez did? Contact The Heaven Solutions today for a comprehensive practice assessment and customized improvement plan. Our proven strategies have helped hundreds of practices achieve similar results through revenue cycle optimization, technology implementation, and strategic guidance.
Don’t wait for a financial crisis to take action. The sooner you begin implementing these proven strategies, the sooner you’ll see improvements in cash flow, operational efficiency, and patient satisfaction. Start your transformation today and secure your practice’s financial future.
